Alumni Recall their First Patient Encounter
What do you remember about your first patient encounter?
- Alumni Rounds
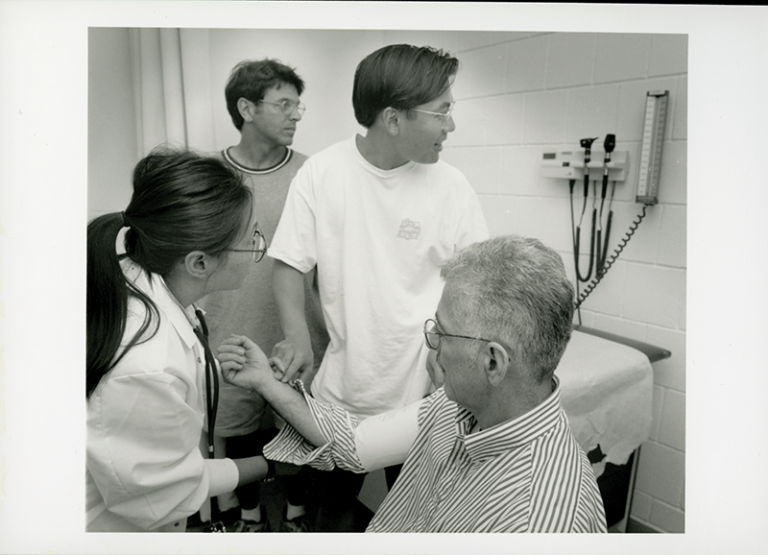
Nneka Azikiwe, MD ’07, examines a patient as Leon Goldman, a former HMS associate professor of surgery at Beth Israel Deaconess Medical Center, looks on. Photo was taken in the late 1990s.

Nneka Azikiwe, MD ’07, examines a patient as Leon Goldman, a former HMS associate professor of surgery at Beth Israel Deaconess Medical Center, looks on. Photo was taken in the late 1990s.
Laurie Green, MD ’76
In our day, inpatient stays were long. As medical students, we had little to add to medical decision-making. However, we had the time by the bedside, and, in turn, the patients taught us humility and humanity. Gilda had lung cancer and died at 34, a nonsmoker with three children. Donnie had congenital heart disease and multiple cardiac surgeries. He lived in Lowell with his mother. I kept up with them until he died at 32. Forty-five years later, I still cherish his drawings and Gilda’s locket.
Laura Holmes, MD ’83
As a first-year medical student, I had a wonderful clinical preceptor, Laurence Green, MD ’72, a cardiologist at the Brigham. My fellow student and I visited an elderly woman with heart failure and listened as our preceptor interviewed her. She denied all claims of chest pain or shortness of breath. Upon further questioning by Green, she disclosed that she sat in a chair or up in bed all day. Later, he told us that a successful clinician puts a patient’s history into a practical context.
Tamara Fountain, MD ’88
During OB-GYN rotation at the Brigham, I was assigned to be an overnight companion for a young expectant mother who was in premature labor and had no one to be with her. We both slept between contractions but talked about everything under the sun when we were awake. In the morning, her husband, having arranged childcare for their toddler at home, arrived to relieve me. I found out later she gave their new baby girl the middle name Tamara.
Samuel (Bob) Snodgrass, MD ’63
I examined patients from the second year on; in terms of doing something for patients I most remember putting patients in casts, reducing a dislocated shoulder, and sewing up simple wounds during my Brigham surgical rotation. I had no interest in going into surgery, but these experiences stayed with me.
Barry Pressman, MD ’67
I was surprised how receptive the patient was to being examined by this obvious neophyte.
Ken Lin, PhD ’08 MD ’10
I had the fortune to get assigned to a very patient patient. My H & P exam must have taken no less than an hour, and it turned into a fun conversation with the middle-aged gentleman. He was an active marathon runner who had been admitted for cellulitis. He had been an ED nurse, so he gave me constructive feedback on my physical exam. The conversation I had with him did inspire me to run the Boston Marathon a year later.
Richard Sogg, MD ’56
I remember being terrified, feeling inadequate to actually deal with a human being, even as one of our group of four leisurely sat on the bed with the patient! That student later became a dean at a dental school.
Peter Barrett, MD ’60
I was a second-year student at HMS in the spring of 1958, assigned to the MGH for physical diagnosis. I can still feel the warm breeze as it came through the open windows of Bulfinch 2, where I met my faculty mentor on the open ward. After some general remarks, he pointed out a frail, elderly woman on the far side of the room. My task was to approach the patient alone and obtain a relevant history. No physical exam was to be performed.
My patient was sitting quietly on the side of the bed and appeared comfortable. I introduced myself and began to ask about her health. Struggling through a review of systems, I learned little except that she did not smoke. My attempts to obtain a family history resulted in a lengthy account about dozens of relatives; I was no longer in control. Notably, she had two older brothers who fought for the Union at Gettysburg and survived. One of her sisters ‘caught the dysentery’ and died, and her parents’ farm had been damaged.
At this point my mentor, my savior, arrived. I could not tell him why the patient had been admitted but could point out that she had had two brothers who fought at Gettysburg.
He asked me if I had noticed anything about the patient that could be of importance, even though I had not been asked to perform a physical exam. I had nothing to report.
Does she smoke? asked my mentor. I felt proud that I had pulled this important information from my patient and told him that she did not smoke. He then turned to my patient: Do you smoke? No. Do you use a pipe? Yes, she used a pipe regularly, a corncob pipe, which lay on the bedside stand. She complained that the nurses would not let her use it on the ward.
While taking care to not embarrass the patient, my mentor continued speaking to her and pointed out an obvious lump on her left lower lip. He also pointed out a subtle fullness on the left side of her neck.
I had missed my first diagnosis, but I learned a great deal about the need for observation as part of the patient encounter, and as a bonus, I learned a great deal about the Battle of Gettysburg.
Richard Moskovitz, MD ’73
In our introductory course on interviewing, I was assigned to interview a renal patient. I proudly presented the detailed results of my interview. Then the instructor asked if there was anything else I’d noticed about the patient. Turns out he was quadriplegic—I’d failed to notice that he hadn’t moved throughout the interview.
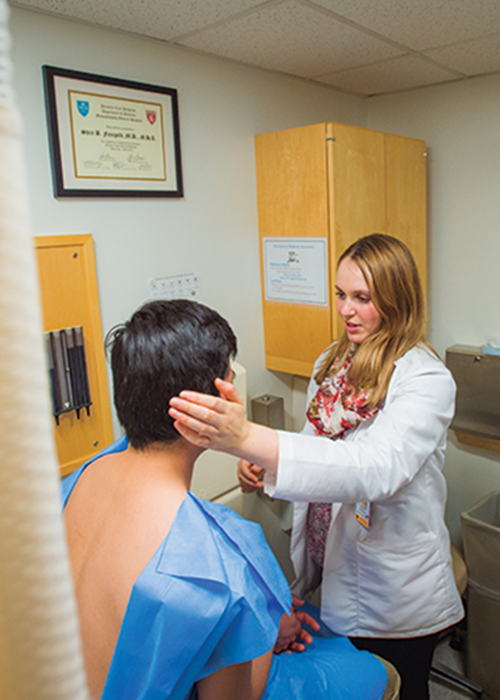
Joseph Savino, MD ’84
It was an AIDS patient, surrounded by the unknown and fear; HIV-1 had not yet been identified. We entered the patient’s room in “astronaut suits,” because we were going into a room with a disease we did not understand. The health care providers were frightened, fearful of contracting whatever it was. I can only imagine how frightened the patient was. A lesson learned long ago, apropos for today.
Kara Wong Ramsey, MD ’09
It was with an elderly patient and my preceptor in my preceptor’s primary care practice. I remember wearing my white coat with pride as I began my interview and feeling like a “real doctor.” I tried to be thorough in my physical exam as we had learned in our didactics, textbooks, and videos, not wanting to miss any small thing. I think the patient was amused by my enthusiasm. I think of that thrill when I precept my own medical students now and see their joy to be at the patient’s bedside.
Martin Prince, MD ’85
It was an elderly patient with basal cell carcinoma of the nose, who was in the midst of a reconstruction procedure where skin from the chest was being brought to the face. He could not really talk to me because his face was tethered to his chest. It was tough to figure out what was going on.
George Hill, MD ’57
It was in physical diagnosis, at the MGH. We had been taught to take a careful history of the present illness, a history of past illnesses, including childhood diseases, and a review of systems. Our group of four second-year students was shepherded by a surgeon, Frank Wheelock, MD ’43. He asked each of us individually to examine one of his patients. When three of us had finally finished, Bob Rivers went in and immediately came out. He made the diagnosis immediately, and later became a great surgeon.
Richard Burney, MD ’69
On the morning of Monday, December 4, 1967, I reported to Boston City Hospital to start the Principal Clinical Year. I was on Peabody 2, the women’s ward. I wrote in my journal at the time: “My first night on call was truly surrealistic. During the course of the evening we had in close succession an acute pulmonary embolus causing ventricular tachycardia, an uncontrollable woman in DTs with a fever of 103 on whom we had to do a lumbar puncture, and a lady with dementia who had aspirated her dinner. It was unreal. It was quite a start.”
Karen Singer, MD ’77
I remember the humanity, actually being with a person who was generous enough to allow a student to interview them.
Peter Schrag, MD ’64
Joel Rutman and I were classmates and partners in the course on physical diagnosis. We examined patients at Boston City Hospital in 1960 as second-year students. At first, we were lost, but slowly we got better. Joel and I had some good laughs and now in our old age we correspond by email between New York and Israel.
George Lewinnek, MD ’67
My father was a family doctor. My first encounters were watching him treat patients. When I was in college, I sat in the kitchen of an elderly man who had developed diabetes. My father explained the disease to him. I remember feeling disoriented; hearing about glucose seemed so remote when delivered in a lecture at college, but now it was being discussed in an everyday kitchen.
Jane Farhi, MD ’81
My first day as an intern was overwhelming. I was at Elmhurst Hospital, a Mount Sinai affiliate, and nothing at HMS had prepared me for how sick the patients were. Two out of three died and the third, a patient from a psychiatric hospital, had viral meningitis and rhabdomyolysis with acute renal failure.
Peter Zawadsky, MD ’68
My first encounter occurred at Boston City Hospital during the Introduction to the Clinic rotation. The patient was a middle-aged man who had developed mitral stenosis as a complication of acute rheumatic carditis. This was my first experience listening to heart murmurs. Larry Seidl Sr., MD ’61, was my instructor.
Priscilla Slanetz, MD ’91
My first encounter with a patient was with a prisoner admitted for bipolar disorder. My preceptor chose me to take a history during Introduction to Clinical Medicine. It was then I realized that I had an ability to connect with people. Even after the patient told me that he hated people with my first name, I remained calm and managed to get him to tell his story. I felt uneasy throughout but took comfort in the fact that two armed guards were nearby just in case the patient lashed out at me.
Steven Jacobs, MD ’80
The first patient I examined in the physical diagnosis course was a woman who’d been admitted with some sort of GI symptoms. Upon examining her rather obese abdomen I palpated a firm mass in her left lower quadrant that had not been reported. Excitedly, I brought in my attending, who palpated a similar mass in her right lower quadrant. I was so jazzed and started thinking about the differential diagnosis. My attending then told me that the masses were her anterior superior iliac spines.
Sheila Hafter Gray, MD ’58
My first patient was the cadaver I shared with three others in first year. I can still envision him. Finding the cause of his death was, as my current students say, awesome.
Richard Burney, MD ’69
At the time, this is what I recorded: “On Friday, January 20, 1967, we were welcomed into the fold of clinicians as Physical Diagnosis got off to a start. It was the mystical laying on of hands … when we see a patient now, we can say, ‘Good morning, I’m Dr. … ’” It was a joy not to go to lab but to walk out of lecture and into the fresh air and look forward to putting in some “real time” with people. A person with a disease is inherently much more interesting than the disease itself.
Robin (Gottdenker) Smith, MD ’88
One of my early patients was at the VA Hospital. He was described as a grouchy man who rarely let medical students draw his blood. Turns out he loved baseball, and I learned early on that if I checked the baseball score before going to draw his twice-a-day levels that he relaxed and told some great stories, which I still remember today. Patients are people first.
Mary Flowers, MD ’78
I remember having sweaty palms and sweat dripping down my forehead! I was fresh from the segregated South and had suffered through the integration of the school system. When I learned that Boston was rioting because of forced integration of the school system, I thought: Here we go again! I inhaled and thought that I would be kicked out of the room because of the color of my skin.
Karl Singer, MD ’67
The first patient I remember was a man with numbness in his hands and deformities in his fingers. It was my first and last patient with leprosy. I think this patient was frequently presented to beginning medical students.
Blair Eig, MD ’83
The first patient I saw was a woman experiencing back pain. I was embarrassed at how long I took, but the patient was incredibly appreciative of the attention to her concerns. At the end she revealed she was “Mrs. Mike” of Mike’s Pastry, and she had cannoli brought over for the clinic. I realized then that no matter how much knowledge I was to gain, it was the compassionate approach to interactions with patients that would be the most important trait I could develop. And the cannoli were great!
Elizabeth Dreesen, MD ’87
The first person I admitted as a clinical clerk in medicine, at MGH, was an AIDS patient whose name I still remember. He was scared and so was the team, myself most of all. I was scared of AIDS, scared of being a bad medical student, and most of all scared of failing him. He died of pneumocystis at 11 a.m. two weeks after admission. After the death and the death paperwork, my resident, Deb Weinstein, MD ’84, sent me home for the day, which was perhaps the most generous act that I experienced at HMS.
Steven Swerdlow, MD ’75
My first patient encounter was at Boston City Hospital, where I was assigned to take a history and do a physical of my patient and then report back to my instructor. Unfortunately, I was unable to rouse the elderly woman, who was lying in a bed in a large ward; I was concerned she had expired. My instructor was barely able to rouse her. I ended up with no history and no physical. I was very anxious already, and this was not a calming situation. I became a hematopathologist.
Images: Center for the History of Medicine, Francis A. Countway Library of Medicine (top and group of four); Gretchen Ertl (Messinger)