Theater Reviews
Long held to supporting roles, women surgeons are now leading and shaping the field
- 21 minute read
- Perspective
According to Preeti John, a Baltimore-based surgeon who gathered essays, poems, and interviews from sixty women surgeons for her book, Being a Woman Surgeon, a surgeon’s life is challenging, requiring not only physical stamina but also “strength of character, balance, careful planning, and a firm commitment to what is important.” These adapted essays from four of the surgeons featured in the book calmly and proudly attest to the truth of her statement.
Musings of an Accidental Pioneer by Kathryn Anderson
I think that I began my road to being a surgeon at the age of six, right after World War II, when my aunt took me and my sister to the newly reopened Manchester Art Gallery. I gazed at a pencil drawing of Theatre by Barbara Hepworth, who is better known as a brilliant sculptor. It depicts an operating room with a table surrounded by mostly men and one woman, undoubtedly a nurse. Nothing changed my mind, although being a woman surgical resident in the 1960s almost destroyed my resolve.
No one in Boston would give me a surgical internship, so I became a pediatric intern at the Children’s Hospital and entered surgery at the residency level at Georgetown. There, getting through the next rotation occupied all my time and energy. Children remained my first love, and I became a pediatric surgeon, one of the first to take the new pediatric surgery board certification exam.

I began my medical training at the University of Cambridge in England and met my American husband there. I had not wanted to go to Cambridge, as Oxford and Cambridge added a year to the training. Most English universities train physicians in five years, right after high school, with no degree until the medical one. Cambridge gave a bachelor degree halfway through medical school, hence the extra year (there were three preclinical and three clinical years). However, fate intervened. The night before my final exams in high school (the “A” levels, without which I could not get into any university or receive a much-needed scholarship), I came down with appendicitis. I missed the exams and had to stay an extra year in high school; the exams were only given once a year. So I took the Cambridge entrance exams for something to do.
Although there was no formal arrangement between the universities of Cambridge and Harvard, they were “kindred souls,” believing that each was the best university in the world. It was difficult to get into Cambridge, particularly from a state high school rather than a private school, but I passed the entrance exam, and they must have liked me. I was only the second in my high school to be admitted there. My husband was already scheduled to enter Harvard Medical School at the second-year level after his two years in Cambridge, so it was relatively easy to follow him a year later. I finished the last three years at Harvard. Once I finished the second year, a nonclinical year, and started to learn clinical medicine, I did not look back.
However, I did run into overt sexism when I told the dean of students that I wanted to do a surgical internship and residency. I was told that women could not be surgeons, and if I even applied, the dean would make sure I did not get any internship in Boston or elsewhere. So I did a year in pediatrics at the Boston Children’s Hospital, a year I very much enjoyed and have never regretted. Said dean obviously forgot his remarks and could never understand why I would never speak to him again.
Residency: oh dear! In the 1960s, it was very much okay to make sexist remarks and be overtly averse to training a woman (“You’ll only get pregnant and quit, wasting a place which could be better occupied by a man.”). There were a few notable exceptions of surgeons, mostly in the community hospitals I rotated to, rather than the university, who were willing to train me. Once I reached my third year of residency, I was good enough that the surgeons fought to get me to assist them and I did more than 600 cases in that one year, having previously done a total of six cases the prior two years. This included resection of an abdominal aortic aneurysm.
Mostly, my fellow residents, who were of course men, were supportive. A minority who resented it when I was given cases they wanted to do undermined me at every opportunity. I was only the third woman to go through the Georgetown residency. By the time I finished as chief resident, a total of five, including myself, were in the program. There were no support systems, only the sporadic support of individual surgeons, and, for me, a constant—my husband, who was an unending source of comfort and encouragement.
Nurses were marvelous. And there was never a problem with patients; they were only too happy to have attention paid to them, and I was a fairly good listener. I have always had the policy of treating the whole family, whether in my pediatric practice or when I was training in adult surgery, and this worked well for me as well as for the patients.
I would like to say that things have improved, and it is now common for women surgeons to combine a successful career with bringing up children. We chose not to have children for a number of reasons, and although I have no personal regrets, I applaud women who are able to manage career and family with all the difficult choices inherent in “having it all.” This is not to say that the playing field is completely level as yet; there is still some way to go. But the time for stridency is gone. It is entirely possible that integration will occur to such an extent that there will be no need to be distinctive as a woman surgeon—just as a surgeon.
Grateful patients always claim their doctor saved their life. In fact it is quite rare to really cheat death on someone else’s behalf. But when it happens it is the most moving experience. For me, one of those rare privileges was when my grandnephew was born with a heart murmur. The neonatologist assured my nephew that the baby could go home, as the defect would close by itself. In the dim recesses of my brain I remembered that a VSD (ventricular septal defect) most often did not present with a murmur at birth. On my advice my nephew insisted that the baby have an echocardiogram; he had critical aortic stenosis, which most certainly would have resulted in early death if he had been forced to go home. My grandnephew is now a lusty lad, who has no idea of the role I have played in his life, nor that he was the inspiration for me to finally write a book that had been in my head for decades. Who Will Hold My Hand? is for parents whose children need surgery, and it is published by the American College of Surgeons.
How have I managed my complicated life? I pass my philosophy on to readers: You walk one step at a time, so you must achieve milestones one at a time, whatever your role in life turns out to be.
Kathryn Anderson ’64 is a retired pediatric surgeon, formerly affiliated with Children’s Hospital Los Angeles, where she was the first woman surgeon in chief. Anderson also was the first woman president of the American College of Surgeons.
Image: Scott Witter
“Surgimom” by Christine Rohde
I hold the bead bracelet in my hand, rubbing the pink and purple sparkly globes and the M-O-M blocks like a sacred rosary. I am about to head into another twelve-hour operation and yet another day without seeing my kids. My daughter proudly gave me her bead creation, and I proudly wear it at work, tucking it into my coat pocket when I head to the OR. All thoughts of the challenges and rewards of my chosen profession are tucked away at that instant as well. My patient and a successful outcome to her cancer reconstruction surgery are my only priority. And that is how it should be, for everyone going “under the knife” should be assured of the commitment of the person whom he or she trusts to cut, to sew, to repair, to heal. And to know that that commitment exists whether it is day or night, weekend or holiday.

Women in surgery have unique gifts to offer but unique sacrifices to make as well. As I go through my career, every year moving faster than the last, I realize that, although I knew how hard it might be, I never knew how fulfilling it could be. I thought I would be a surgeon even when I had no idea what that meant. My mom saved my elementary-school writing—oversized letters on thin paper with wide lines—“I want to be a doctor someday, maybe a brain surgeon.” I still don’t know where I got that idea. No one in my family is a doctor, let alone a surgeon. Maybe it was just because it seemed like the hardest thing to do. I barely wavered in my path to medical school. Once there, I realized that nothing appealed to me like surgery. I usually advise students that, if there is anything they would like to do in medicine besides surgery, they should probably do that. But for me, there was nothing else.
So I went on to general surgery residency, which, come to think of it, is a lot like delivering a baby: 120-hour work weeks and sixty-hour power weekends, pre-rounding at 3:00 a.m., passing people coming home from a night out. If I try hard, I can remember some of those tough times, but mostly I remember being part of a team; wanting to be nowhere else; learning to be at my best at all times of day or night, no matter how little sleep I’d had; and the overall sense of accomplishment. So, like childbirth, I don’t remember the pain; I only appreciate the good that came out of it.
I never really thought about having a family, other than my family of surgical residents. I did manage to sing in one opera during residency, playing Zerlina in Mozart’s Don Giovanni. Several of my surgical mentors came to the performance, and it was wonderful to see them in another context.
I got married during residency but waited until after finishing plastic surgery residency to have children. There is, of course, no right time for a female surgeon to have kids. I remember hearing the regret of some surgeons who said they waited too long and were never able to have children. I also remember how hard it was for already-overstretched residents to cover for fellow residents if the need ever arose.
Now, years later, I realize that balance is not possible. It is possible to be a great mom and a great surgeon, a great wife, and a great researcher. But balance is not possible. One day, the scale will be tipped more on one side; the next day, it will tip the other way. You can end up feeling off balance and torn.
I am only able to do what I do because of a supportive spouse and family. My husband works as hard as I do, both at work and at home. My mother, who helps with my children, thinks of it as her contribution to my patients, to enable me to work early and stay late. In this regard, we are the same as our male colleagues with families. It is only with the support of others that we can do what we do. (However, I doubt that most of my male colleagues worry about packing school lunches or cleaning toilets when they get home.)
What are the challenges? Being torn between work life and home life. Feeling like I could always do more in one place or the other. The drive to work harder than everyone else, so that no one can ever complain about female surgeons.
And the rewards? The hugs I get from patients. The tears of gratitude. The knowledge that at the end of the day (even if that is the middle of the night) someone has been positively affected by my hard work. I don’t have to wait for a medication to kick in or a laboratory test to come back—I see it at the end of an operation done well.
What’s more, I get to go home to the rewards of kids running around yelling “Mommy’s home,” or a sleepy, soft, post-bedtime kiss.
Mommy’s home. And I get to do it all again tomorrow.
Christine Rohde ’99 is an assistant professor of clinical surgery at Columbia University.
Image: Flynn Larson
Woman Surgeon—From Boston to Baltimore by Sheri Slezak
I first fell in love with anatomy when we dissected a mink in seventh-grade science. Most kids liked the fur. I liked the heart and the intestines. The next thing I knew, I was in Harvard Medical School.

At Harvard, 30 percent of my class was female—a great feat in 1980. I did surgery as my first clinical rotation to get it out of the way, because I definitely didn’t want to be a surgeon. But who knew that it would be so much fun to do a physical exam on someone, then cut them open to see if you were right? Anatomy really is beautiful. The only role models in surgery were a woman cardiac surgery resident who packed a gun in a shoulder holster, and a pediatric surgery resident who consistently managed to alienate people every time she uttered a sentence. Considering this, it was pretty worrisome to want to go into surgery. A rotation in plastic surgery with Joseph Murray ’43 taught me that you can be humble and kind and still be a surgeon.
I did general surgery residency training at Columbia Presbyterian. I was the only female in my intern group of twelve, but there were four women residents in general surgery and orthopedics. We had informal “girls’ surgical service” dinners and supported each other. I was the fifth woman to finish general surgery. Columbia is a great teaching institution.
I interviewed for a plastic surgery residency at Johns Hopkins Hospital. There, they told me about previous women who had left, told me that I could never have babies in their program, and that they had never had a good woman resident. During the interview session, I was sent to lunch with the chair’s secretary. One of the general surgeons there was often heard to proclaim that “Women do not belong in surgery.” It was like going back in time fifty years—or maybe a hundred. Nevertheless, I needed to be in Baltimore, so I signed on. You can learn anywhere, I told myself.
I had my first child in my research year. I told my chair about a cute thing that my child did, and he looked at me and said, “I hate babies.” So he missed out on all the stories about my brilliant infant.
After nine years of training, I took a job as attending plastic surgeon at the University of Maryland and have been here twenty-five years. I had my second child at the age of forty. I asked the Maryland chair of surgery about the maternity policy and he said he would have to get back to me. He called in a week and asked what I wanted it to be. I was surprised that they did not have to close the hospital while I was away for six weeks of maternity leave, but everything seemed to run well without me—a good lesson for me!
My third child was born when I was forty-two years old. It was always a dilemma how to position myself in relation to the OR table: Did I place my ever-expanding belly below it or above, so I could rest the baby on it? I learned that sitting down occasionally during surgery helped my legs a great deal. Ralph Millard always said, “Why stand when you can sit while operating?”
I eventually became a full professor and chair of plastic surgery. Now that I am chair, I can tell you that men ask for a higher salary and a promotion every other month.
We recently had a picture taken of twenty-three women surgeons at the University of Maryland, and many have had children. I am enthusiastic when my faculty members are pregnant. It all works out.
I am proud to be a surgeon. I learn every day from my patients, but my proudest moments are still as a mother of three.
Sheri Slezak ’80 is a professor and head of the Division of Plastic Surgery at the University of Maryland School of Medicine.
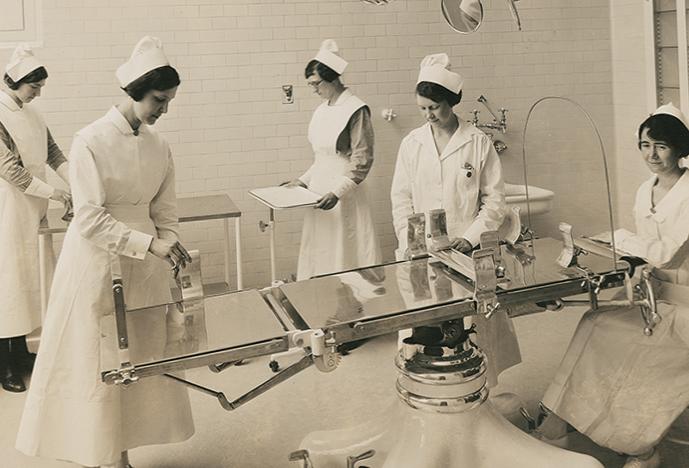
Image: Eli Meir Kaplan; top image Courtesy of Spectrum Health System Archives © 05.2016
“Life is what happens to you while you’re busy making other plans.”
by Susan Pories
First, I planned to be a teacher, then an obstetrician, then a general surgeon, then a trauma surgeon, then a colorectal surgeon, and finally I found my place as a breast surgeon, a writer and a medical educator. I remember going to a lecture entitled Female, Flexible and Fearless; this really resonated with me, and it is important to remember that as you grow and change your goals will too.
I fell in love with Vermont when visiting friends in college, and then transferred to the University of Vermont (UVM) as a junior. At the time, I was planning to be a high school art and English teacher. I taught reading to migrant workers in New York, but the job market for teachers was very competitive at the time, and it was common for 200 people to apply for a teacher’s aide job position. I noticed that teaching jobs were often victim to town budget woes and decided to change directions.

I wanted to be a doctor but was convinced I probably wasn’t smart enough to handle the required science. But to explore this further I took a job as a medical assistant in an obstetrics and gynecology office. I weighed patients, took hematocrits, measured vital signs, washed instruments, filed charts and cleaned exam rooms.
At night I worked in the Burlington Free Clinic, where lay people were trained to follow short protocols for the care of common problems, mostly sexually transmitted diseases. We performed throat and vaginal cultures. We learned to do procedures by practicing on each other. I was a nervous wreck the first time I did a vaginal exam, but my co-worker and friend Joannie put me at ease, saying, “I’ve had two kids, Susan. I have a big, baggy vagina. You can’t hurt me.” I relaxed and all went well.
Most of the clinic volunteers were interested in applying to medical school and did so successfully. One day, Gary Z. came to the obstetrics and gynecology office where I was working to shadow one of the doctors. As a medical student, he was treated like royalty. The doctors showed Gary interesting findings under the microscope, took him in to examine patients, and spent time talking with him about physical findings. Since I knew Gary from the clinic, I knew that I was his equal; and it was on that day that I made the decision to go to medical school. My plan at the time was to be an obstetrician, just like the doctors I worked for. I had no money from my family at that point, since they had made a decision not to pay for graduate education. No matter. I quit my job, took out loans and signed up for pre-med classes, calculus, physics, chemistry, biochemistry and biology. When I finished the courses and took the MCAT exams, I applied to medical school and took a job in a research lab at UVM. We were studying the actions of prostaglandin in monkey ovaries.
UVM was my first choice for medical school because I loved Vermont, was a state resident and qualified for more reasonable tuition. In addition, I met my husband in Vermont and his family was in the area. He didn’t really want to go to another state. The interview at UVM was weighted heavily, and I was very anxious about this. I was interviewed by a fourth-year medical student and primary care doctor, Mildred Reardon. I have forgotten most of the details, but do remember that they asked me what my strengths were. I answered that my strength is that I’m strong, meaning that I always show up and get the job done. I berated myself after the interview for giving a dumb answer. My strength is that I’m strong. What a stupid thing to say! But, as it turns out, Dr. Reardon gave me a “thumbs up” and I was accepted.
Actually, being “strong” is one of the most important qualities for a career in surgery. You do need to be physically strong and have a strong ego and a strong work ethic, just to keep going and show up every day without fail—even if the patient is not doing well, even if you don’t feel well, even if you made a mistake, even if you don’t get the promotion you want. … No matter what happens, being a surgeon is a responsibility that is with you twenty-four hours a day, seven days a week. Once you take responsibility for a patient, then you have to do your best for them and be there for them.
I was very lucky to be accepted at UVM, a very clinically oriented medical school where the culture has always been that the patient comes first. And UVM was one of the first departments of surgery to accept and graduate women surgeons. The chairman of surgery at the time was Dr. John Davis. Dr. Davis was one of the first surgical leaders to actively and consistently mentor and support women in surgery. At a time when most programs refused to consider women for surgical residency, John Davis not only accepted women residents but made sure that women were treated fairly. As chairman, he supported women in surgery and treated them as equals. Unfortunately, in 1986, Dr. Davis was stricken with viral transverse myelitis, which left him paralyzed from the chest down. He was forced to step down from his position as chair of the department. Although officially retired, he remained an active educator for many years. With a sharp wit and intellect and a ready sense of humor, he was a role model for many surgeons. In 1991, the American College of Surgeons bestowed on Dr. Davis their highest honor, the Distinguished Service Award.
Surgical training was tough by any standards. There were no work-hour restrictions in place at the time, and programs were traditionally pyramidal, meaning that more people were hired at a junior level than could graduate. This meant that at least one person had to be “cut” every year. This had the effect of discouraging complaining and pushing everyone to do their best, but also took a toll on relationships between residents. Pyramidal programs have been discontinued, and now residents who are “categorical” are guaranteed to finish their training, provided that they meet all the requirements of training. Work-hour restrictions have also improved the quality of life for residents today. However, when I was a resident, any discussion of an easier schedule implied you were weak—and nobody wanted to be perceived that way. In fact, the “best” programs were every other night call, because call every third night meant you were missing too many good cases.
The program in Vermont was very strong in trauma training, because Dr. Davis was a MASH surgeon in the Korean War, and was internationally recognized as an expert in trauma care. Several other surgeons in the department served in Vietnam as well. Trauma cases came to UVM Hospital from all over Vermont, as well as parts of New Hampshire, New York, and Canada. Naturally, I wanted to be a trauma surgeon in the beginning. Over time I became more interested in cancer surgery, and after residency I moved to Boston for a surgical oncology fellowship. This was focused on colon cancer research and I was hoping to be a colorectal surgeon. However, at the same time, I had my son and that really changed my perspective. A colorectal fellowship would have required moving and more time away from my family, so after the oncology research fellowship I went into practice. At first I did all kinds of general surgery cases, but over time my focus became breast cancer, both clinically and from a research perspective. Now I can’t imagine doing anything else, and feel that I have been very lucky to have great mentors and opportunities along the way in my career. One of the keys to success in surgery or any other field is to be flexible and resilient. Remember not to give up when things don’t happen the way you first imagined.
The title of this essay is from John Lennon’s song “Beautiful Boy (Darling Boy).”
Susan Pories is an HMS associate professor of surgery and medical director of Mount Auburn Hospital’s Hoffman Breast Center.
Image: John Soares
Essays are adapted from Being a Woman Surgeon: Sixty Women Share Their Stories, edited by Preeti R. John, with permission from the publisher, Gordian Knot Books/Richard Altschuler & Associates, Inc., Los Angeles, California